反思COVID-19: 重新思考医疗服务正当时

随着我们逐渐从新冠流行病的危机中恢复,SmithGroup开始设计解决方案,控制医院和企业在回归“正常”的过程中控制疾病感染。但是,医疗环境会恢复正常吗?还是会产生新的情况?
这次疫情给我们的医疗保健系统带来的严重冲击。未来将会有数以百计的论文和研究来讨论应对能力、医疗服务获取和公平性、公共卫生以及整个医疗系统当中的问题。但首当其冲的,是及时和积极地应对感染控制问题,这样才能有利于病患者在新冠疫情消退后安全重返医疗设施就医。
所有类型的医院和护理设施都需要对患者和工作人员的安全做出明确安排,以减轻他们在这些方面的担忧。SmithGroup 医疗团队正在探索几个新的有利于保障这种安全的概念及其对它们对医疗环境的影响。我们的研究显示,医疗设施有必要在技术、流程、人员和场地四个方面改进,以应对后疫情时代的新需求。
这些想法旨在创建一种新的整体护理模式,方便患者就诊,限制潜在感染,并专注于使医疗保健系统回到正轨,同时确保患者和员工的安全。
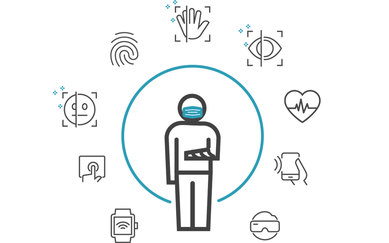
技术
"尽量不要外出"已成为医疗保健业的新口号。在美国,护理提供者和患者出于必要开始以前所未有的态度接受远程医疗和家庭护理。这种在 COVID-19 危机期间形成的短期解决方案也是帮助患者就医和减少感染传播的长期解决方案。为了有效地将远程医疗纳入护理模式,我们需要制定更具战略性的规划和设计方法,以调整设施规模并限制过度建设。
探索健康管家
- 带监控的可穿戴设备
- 远程咨询/门诊
- 远程护理协调员,确定最安全的护理方式
- 在家咨询、送药上门、监测设备、康复
- 集中式护理协调资源(流程一致、患者回访、健康管家)
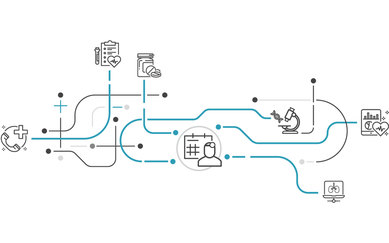
流程
技术、流程和设施必须协同工作。免接触的医疗设施解决方案未来将成为标准做法。免接触的概念对环境和流程有要求,以减少或消除患者和员工接触家具、固定装置和设备的需要。新的患者就医路径将产生,以限制患者和访客聚集,并帮助医疗过程简化和流畅开展,从而减少流线交叉和潜在的感染可能性。工作人员安全区将为护理提供者提供改善空气质量的解决方案并减少传染风险。
机器人可用于无接触物流以及清洁和维护。预约和挂号的技术将使患者能够通过在线网站或应用程序在家中完成基本信息填写,无需患者和员工在每次就诊时触摸可能受污染的登记板、笔和电子设备。
探索患者寻路设计
- 支持人工智能的应用,用于输入症状并确定理想的就诊路径
- 为到访患者提供最近预约时间(患者导航员)
- 将患者直接引至最安全的设施入口/就诊路径:限制穿过长走廊和可能污染的区域,借用购物街的概念,以洁净走廊串联各科室
- 感染控制管理设施评级
改善运营流程(如接诊量)也有助于防止感染传播。让需要与医生当面接触的患者自助进入检查室可以去免去病人在候诊室停留,和接触受污染的家具和设备的风险。
探索远程签到
- 免接触挂号,远程签到和积极的动态更新
- 通过数字设备进行自助进入检查室
- 可穿戴设备,将监控和诊断数据直接传输到患者的电子病例
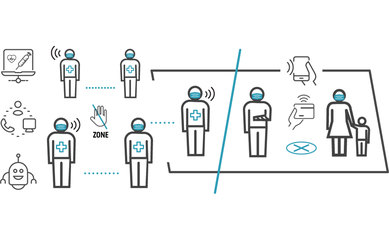
人员
建立安全的员工区对于降低护理人员感染的风险至关重要。现有的前台/后台设计概念是一个开始,但清洁的核心工作环境需要更高的要求。这一概念提供了指定的、无病人进入的员工区域(后台),这些区域由先进的机械系统支持,能提供更清洁、更安全的环境。
探索员工安全区
- 家庭和远程医疗监测站点的后台安全中心(虚拟护理中心)
- 改进医疗保健设施内的员工安全区的机械系统(湿度控制、空气治疗系统、额外的外部空气)
- 建筑分区,以限制人流量并根据需要设置隔离区
场地
建筑设计可通过为门、灯和其他设备提供传感器控制来支持无接触概念,无需工作人员和患者通过建筑环境进行交叉感染。
探索免接触设施环境
- 无接触患者检查路径:无等待、自助进入检查室、自动门
- 工作人员的后台协调区域:争取实现患者就诊、自动门之间、语音控制文档或远程记录的零接触
- 100% 感应水龙头(无接触水槽),具有有效的定时机制,用于感染控制; 动作或语音控制(温度、照明)
现在到了为了医院恢复运营而设计的时候了。SmithGroup 团队正在努力创建一个可行、全面和积极的未来设施规划和设计战略:技术、流程、人员与地点的精心设计集成,使我们能够创造医疗保健的"新常态"。
医疗保健行业从未有过这样的机会来重新思考如何提供服务。我们是要照旧恢复正常业务,还是主动抓住这个机会,讨论如何重建医疗保健,迎接下一代的医疗挑战?