Leaving Old Habits Behind: Transition Planning Ensures Space Operates as Designed
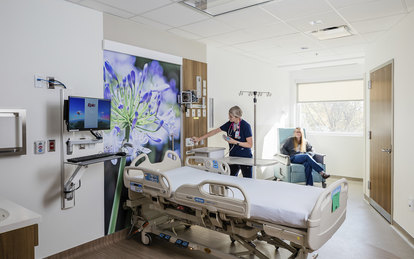
The planning and design of any new or renovated healthcare facility can be a catalyst to change or improve a facility's operating model, just as a change in an operating model often drives the need for new space. In every project, healthcare planners and designers collaborate closely with users to make sure the design and operations work together: that both function as intended. Yet, when staff finally move-in to a new space, the operational intent of the physical design is often poorly communicated or forgotten entirely. Why does this lost opportunity happen, and how do we ensure expectations are met?
During the planning and design phases, there are ongoing discussions about best practice models and opportunities to improve operational efficiency. The design is developed based on many cross-disciplinary ideas for improvements, and then months, sometimes years, go by until construction is completed, and move-in day arrives. Over that time, the clinical staff often changes, the design team has moved on to new projects, and the original operational design intent is sometimes left without champions. This creates the conditions that allow old habits from old spaces to move into the new building.
We can, however, break this cycle. New facilities cost a lot of capital, take a lot of time, and require intense coordination. Providers spend millions of dollars on facilities; it's critically important to know how a building works. You get instructions manuals for everything these days—cars, microwaves, cell phones—why wouldn’t you need one for your complex medical facility?
Transition Planning is a process for evolving a set of existing operational patterns to align with a new care environment—leaving old habits in old space. It is related to but should not be confused with move management, which is the logistical process of moving furniture, fixtures and equipment (FF&E), as well as patients. Transition Planning is essentially the operating manual for the new space: it documents not just how things should work, but why.
Process Investigation
Transition Planning focuses on the future-state flow of patient, staff, and materials within and between departments; processes and standardization within the care environment; and staff training and education. Beginning with a process investigation phase, these multi-disciplinary areas of focused improvement are outlined for various scenarios and used to inform the new space design as well as the operating model. The outcomes of this process investigation create a comprehensive structure for transition planning.
The goal of transition planning is to envision the ideal experience by defining the ideal process for each patient interaction, breaking down departmental silos, and focusing on the total experience from the perspective of the patient. Each defined activity is then overlaid with the new space design and multi-disciplinary processes are outlined for various scenarios, ranging from emergency response drills to testing new communications systems and equipment.
As an example, for a recent hospital expansion and renovation project, one of the owner's goals was to create a safe environment for mental health patients entering through the emergency department (ED). A new suite was created on the floor above the ED for emergency assessment and treatment. As move-in day approached, the SmithGroup transition team came forward to discuss the implications of the new space with clinical and support staff. As we walked through each workflow, a question arose about how security, stationed on the floor below, should access the new space after-hours if an escalation event occurs and their help is needed. The dietary team also needed to determine how the unit was going to be served throughout each day. It quickly became apparent that an access and communication plan needed to be in place before opening. Together, the transition team and unit staff established new protocols for when and how the unit was opened or closed during peak and valley volumes, which were then documented in the Transition Manual. Revised elevator resting locations were programmed into the vertical transport system to allow expedited access to the new floor, a solution that might not have been identified without thorough transition planning.
A Manual to Guide Change
Clinical teams will be accustomed to the operational model that fit the space they were in, and often assume they will continue functioning the same way in a new space. A transition planning team is able to virtually walk clinical and support staff through their operations to test scenarios and create protocols for multiple likely conditions prior to move-in.
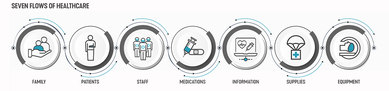
SmithGroup structures this process on the seven flows of healthcare—family, patients, staff, medications, information, supplies, and equipment—working with teams for each functional area to revisit and refine the ideal processes to put in place once construction is complete. We typically begin by working with the patient experience team, who are on the front line of addressing the overall patient experience. Discovering themes of patient concerns in an existing area creates a solid framework for process improvement when moving into a new space. This gives the clinical team confidence in the changes, knowing that they are armed to deliver a safe and positive patient experience that reflects the quality and intent of the new design. This testing and refinement process then continues for all clinical and support teams. A comprehensive Transition Manual, organized into the seven flows, documents these changes and scenarios. Armed with this manual, staff can begin to learn, train—and mentally adjust—to operational changes.
Our transition planners recently met with a patient experience team to outline each of the seven flows for a new patient tower. Because food service was cited as the number one patient complaint, we reviewed the existing process and time for tray delivery and overlaid that data with patient feedback. After discovering that specific floors consistently had more complaints, we shadowed nutrition services and floor staff as they delivered trays over each shift. Our observations revealed that these floors received the earliest trays, around 11:00 am, but that these units also admitted and discharged the majority of their patients between 11:00 am and 1:00 pm. Trays were sitting for up to two hours while staff were occupied with patients. The team revised delivery times for when nurses are less engaged with rounding, discharge, and admissions, and new travel paths were mapped and coordinated for faster delivery. These changes were documented in the transition manual, and the staff was trained in the new processes before the tower opened.
Move-In Day
Just before move-in day, we tour the staff through their new space, building excitement for their new workplace and what their patients will soon get to experience. The transition planning team is on-site to walk staff through each process modification plan in their manuals. Together, teams run through "day in the life scenarios," working through any last questions as they gear up to greet the first patient. The clinical staff are less anxious, knowing they are prepared for this change. On move-in day, patients will experience an organized transition; staff will know how to adjust operations in the new space and a usually chaotic move goes more smoothly.
Because a comprehensive and planned structure was proactively put in place and documented, old habits were left behind, and new practices and procedures are adopted. Using this process, we typically see both patient and staff satisfaction scores improve substantially.
Whether activating a clinic, a single unit, or an entire hospital, an integrated and precise transition plan can ensure that the original goals and design intent of the new space are met. A well-documented and tested plan also ensures that staff and patients are supported, and all staff are trained and comfortable with their new physical environment, workflows, processes, and technologies—and, most importantly, that there is a smooth transition from old to new.